Trials
Trials are the operational spine of TrialStack — they hold study identity, eligibility, scientific structure, and every connected record teams need to plan, execute, and govern a clinical study.
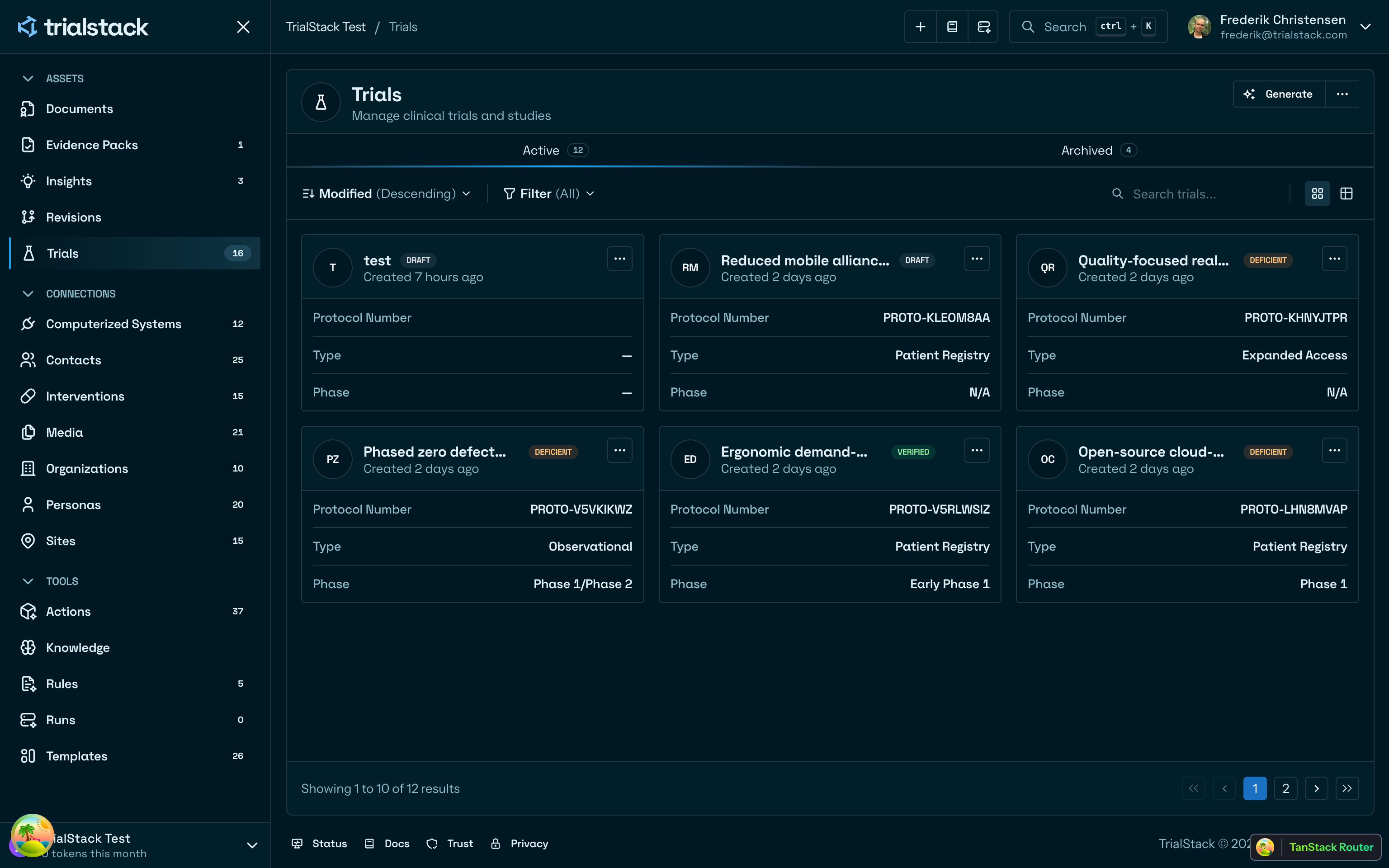
Run the study from one record
flowchart LR
Scattered[Scattered study context] --> Trial[Trial record]
Trial --> Design[Design and start-up decisions]
Trial --> Context[Connected operational context]
Trial --> Governance[Governed review and history]
Teams rarely fail because they have no study data. They fail because study context is scattered across documents, spreadsheets, and memory with no single governing anchor.
A trial record gives the team one durable place to answer questions such as:
- what is this study, who is it for, and what does it measure
- which organizations, sites, contacts, and interventions participate
- what eligibility criteria, endpoints, and objectives define the scientific structure
- whether changes to the study are traceable and reviewable
That matters because almost every other record in TrialStack — organizations, sites, contacts, interventions, personas, media, systems — becomes operationally meaningful only once it is connected back to the trial it supports.
Keep context connected
flowchart LR
Trial[Trial] --> Orgs[Organizations]
Trial --> Sites[Sites]
Trial --> Contacts[Contacts]
Trial --> Interventions[Interventions]
Trial --> Personas[Personas]
Trial --> Systems[Systems]
Trial --> Media[Media]
Trial --> Modules[Specialized modules]
Modules --> Workflows[Design, review, and start-up workflows]
TrialStack treats the main trial record and the specialized trial workflow modules as related but different surfaces.
- the main trial record holds the cross-study description, classification, criteria, objectives, outcomes, identifiers, and all entity relationships
- the specialized modules hold deeper operational work such as design, approval, monitoring, recruitment, retention, safety, schedule, engagement, and statistical detail
That split matters because teams can keep one clear study anchor without forcing every trial-facing workflow into one overloaded form. The main record is the study-wide spine; the modules are where discipline-specific work deepens.
Teams usually get the most value from the trial record when they need to make cross-cutting study decisions, not when they are producing background documentation.
The page is especially useful when a team needs to:
- establish the foundational study identity before connecting sites, contacts, and interventions
- define the eligibility framework — indications, inclusion, and exclusion criteria
- structure the scientific measurement model — endpoints, objectives, estimands, outcomes
- frame the risk–benefit justification and treatment context
- maintain governance across changes with full version history, compare, and restore
Trials also connect in both directions. A team can start from the trial and connect relevant entities, or start from an organization, site, or intervention and link back to the study it supports.
On the page
The trial page is section-based rather than flat. It is built around fifteen governed sections, with specialized modules and relationship tabs alongside.
| Surface | Purpose | What users do there |
|---|---|---|
| Summary | Maintain the study-wide description and structure | Capture identity, classification, criteria, endpoints, objectives, estimands, outcomes, identifiers |
| Trial modules | Hold deeper operational work by discipline | Move into design, approval, monitoring, recruitment, retention, safety, schedule, statistical, engagement |
| Relationship tabs | Keep operational context visible | Review linked organizations, sites, contacts, interventions, personas, systems, media, documents, evidence packs |
Most teams use the page in a rhythm like this:
- Create the trial record and establish the study identity.
- Define eligibility criteria, endpoints, and objectives.
- Connect organizations, sites, contacts, interventions, and personas.
- Move into specialized modules as planning and execution deepen.
- Review history, compare versions, or restore earlier states when the change path matters.
flowchart TD
Page[Trial page] --> Summary[Summary sections]
Page --> Modules[Trial modules]
Page --> Relationships[Relationship tabs]
Summary --> Core[Identity, criteria, objectives, outcomes]
Modules --> Discipline[Design, approval, monitoring, recruitment, retention, safety, schedule, statistical, engagement]
Relationships --> Context[Organizations, sites, contacts, interventions, personas, systems, media, documents, evidence packs]
A strong trial record is not just a protocol paraphrase. It gives the team a governed study anchor they can actually make cross-cutting decisions with.
Good trial records usually do six things well:
- they establish a clear study identity with title, protocol number, phase, and design classification
- they define eligibility criteria that are specific enough to be operationally useful
- they structure the scientific measurement model so endpoints, objectives, and estimands remain explicit
- they keep the risk–benefit justification visible and connected to treatment context
- they connect every relevant entity — org, site, contact, intervention, persona, system — so operational context is never orphaned
- they preserve a traceable change history because trial modifications have downstream impact
That is why only Title is required. The point is not to force completion of every section. The point is to capture the information that supports real downstream decisions.
Review, history, and other governed behavior are covered in the Workflows section and apply here in the same way they do across the rest of the governed record model. All fifteen sections support verification status tracking.
Overview
This section establishes the foundational study identity. It is the first thing reviewers see and the anchor for every downstream section.
| Label | Description | Type |
|---|---|---|
| Title | The primary study title that identifies this trial across the system | Text |
| Protocol Number | Formal protocol identifier used for regulatory submissions and cross-system reference | Text |
| Responsible Party Type | Who holds responsibility for registration and reporting | Select |
| Study Type | Whether the study is interventional, observational, or another design category | Select |
| Phase | Clinical development phase that frames the study scope | Select |
| Primary Purpose | The main scientific objective — treatment, prevention, diagnostic, or other | Select |
| Interventional Study Model | Design structure such as parallel, crossover, single group, or factorial | Select |
| Control Type | What the study compares against — placebo, active comparator, dose-comparison, or other | Select |
| Enrollment Count | Target number of participants the study plans to enroll | Number |
| Masking | Whether the study uses single-blind, double-blind, open-label, or other masking approaches | Select |
| Masked Roles | Which roles are masked — participant, investigator, outcome assessor, care provider | Multi-select |
| Therapeutic Areas | Disease or therapy categories the study addresses | Multi-select |
| Synopsis | High-level study summary intended for quick orientation | Rich text |
| Background and Rationale | Scientific and operational rationale that justifies the study | Rich text |
Risks
This section captures the known potential risks that should remain visible as part of the risk–benefit justification.
| Label | Description | Type |
|---|---|---|
| Category | Risk classification such as medical, procedural, or psychological | Select (badge) |
| Title | Short identifier for the risk | Text |
| Description | Detailed explanation of the risk and its context | Rich text |
Benefits
This section captures the known potential benefits that balance the risk profile.
| Label | Description | Type |
|---|---|---|
| Category | Benefit classification such as therapeutic, diagnostic, or quality-of-life | Select (badge) |
| Title | Short identifier for the benefit | Text |
| Description | Detailed explanation of the benefit and expected impact | Rich text |
Reference Therapies
Reference therapies frame the treatment context by identifying comparator treatments, standard-of-care references, or rescue medications.
| Label | Description | Type |
|---|---|---|
| Linked Intervention | Optional link to an intervention record for cross-referencing | Combobox |
| Therapy Type | Whether the therapy serves as comparator, rescue, standard-of-care, or other | Select (badge) |
| Rationale for Selection | Why this therapy was chosen as a comparator or reference | Rich text |
| Dose Rationale | Justification for the dosing regimen | Rich text |
| Frequency | How often the reference therapy is administered | Text |
| Duration | Length of the reference therapy period | Text |
| Supply Source | Where the reference therapy is sourced | Select |
| Notes | Additional context about the reference therapy | Rich text |
Medication Restrictions
Medication restrictions define which medications participants must avoid and under what conditions.
| Label | Description | Type |
|---|---|---|
| Name | Medication or therapy name | Text |
| Category | Restriction classification such as prohibited, conditional, or washout-required | Select (badge) |
| Washout Period | Required washout duration before study participation | Text |
| Rationale | Why this restriction exists and its scientific justification | Rich text |
Indications
Indications identify the medical conditions or disease areas the study targets.
| Label | Description | Type |
|---|---|---|
| Name | Indication or condition name | Text |
| Is Primary | Whether this is the primary or secondary indication | Toggle |
| Description | Additional context about the indication and its relevance | Rich text |
Inclusion Criteria
Inclusion criteria define who is eligible to enter the study.
| Label | Description | Type |
|---|---|---|
| Text | The full inclusion criterion statement | Rich text |
Exclusion Criteria
Exclusion criteria define who should not be enrolled in the study.
| Label | Description | Type |
|---|---|---|
| Text | The full exclusion criterion statement | Rich text |
Endpoints
Endpoints define the specific measurements the study uses to evaluate outcomes.
| Label | Description | Type |
|---|---|---|
| Title | Name of the endpoint | Text |
| Level | Whether primary, secondary, or exploratory — filterable across the table | Select (badge) |
| Data Type | Nature of the measurement such as continuous, binary, time-to-event, or categorical | Select (badge) |
| Description | Detailed specification of what the endpoint measures and how | Rich text |
Objectives
Objectives state the scientific questions the study is designed to answer.
| Label | Description | Type |
|---|---|---|
| Name | Short objective title | Text |
| Level | Whether primary, secondary, or exploratory — filterable across the table | Select (badge) |
| Description | Full objective statement with context | Rich text |
Estimands
Estimands define the treatment effect the study intends to estimate, following ICH E9(R1) guidance.
| Label | Description | Type |
|---|---|---|
| Name | Short estimand title | Text |
| Level | Whether primary, secondary, or exploratory — filterable across the table | Select (badge) |
| Description | Full estimand definition including population, variable, intercurrent events, and summary measure | Rich text |
Discontinuation Criteria
Discontinuation criteria define the conditions under which a participant or the study itself may be stopped.
| Label | Description | Type |
|---|---|---|
| Title | Short name for the discontinuation criterion | Text |
| Scope | Whether the criterion applies at participant or study level | Select (badge) |
| Category | Classification such as safety, futility, efficacy, or administrative | Select (badge) |
| Estimand Strategy | How this intercurrent event is handled in the estimand framework | Select |
| Is Mandatory | Whether discontinuation is required or discretionary when the criterion is met | Toggle |
| Description | Full explanation of the criterion and its operational implications | Rich text |
Subject Replacement Rules
Replacement rules define how and when participants who discontinue can be replaced to maintain study power.
| Label | Description | Type |
|---|---|---|
| Title | Short name for the replacement rule | Text |
| Trigger Criterion | Which discontinuation criteria activate this replacement rule — cross-references the Discontinuation Criteria section | Multi-select |
| Replacement Window Value | How long the replacement window stays open | Number |
| Replacement Window Unit | Time unit for the replacement window | Select |
| Max Replacements | Upper limit on how many replacements are allowed under this rule | Number |
| Description | Full explanation of the replacement logic and any constraints | Rich text |
Outcome Measures
Outcome measures define registry-facing measurements used for reporting and compliance.
| Label | Description | Type |
|---|---|---|
| Title | Name of the outcome measure | Text |
| Type | Whether primary, secondary, or other | Select (badge) |
| Time Frame Value | Measurement window duration | Number |
| Time Frame Unit | Time unit for the measurement window | Select |
| Description | Full specification of what is measured and how | Rich text |
Secondary Identifiers
Secondary identifiers capture external reference numbers used for cross-system tracking and regulatory submissions.
| Label | Description | Type |
|---|---|---|
| Identifier | The external identifier value | Text |
| Type | Kind of identifier such as registry, regulatory, or internal | Select (badge) |
| Domain | Which system or domain the identifier belongs to | Select (badge) |